RetinaLink Series Staying the Course is pleased to feature Dr. Audina (Nina) M. Berrocal today. Dr. Berrocal is a Professor of Clinical Ophthalmology at Bascom Palmer Eye Institute (BPEI) in Miami, FL. She operates at BPEI and Jackson Memorial Hospital.
Dr. Berrocal describes her clinic and surgery days in our new normal of the COVID-19 crisis. She provides insight into her PPE protocol, changes in her operating room and what she is doing to relieve stress during these extraordinary times.
RetinaLink (RL): How many patients are you seeing each day? What surgical procedures are you still doing?
Audina (Nina) Berrocal (NB): I am seeing approximately 10-20 patients a day (ARMD and diabetics for injections; ROP and post-ops (both kids and adults). Some patients want to come in, others like a phone call and the younger patients like a video chat appointment. There is also quite a bit of emailing and texting photographs with eye concerns, but I am not surprised that many patients just need to talk and the many times we do talk about the crisis and how to protect ourselves. I continue to perform ROP screening and treatment as always. The only change in ROP screenings is that we do not bring residents, fellows or medical students. At this time, we are limiting exposure for everyone in the NICU.

Dr. Berrocal with her clinical team
In the operating room, I have only done cases that have to be done: retinal detachments in both adult and children. Any kids who are in the midst of treatment such as FEVR, IP, COATS (especially if any of these are monocular kids) continue treatment. When this all started, I had just done the first eye of a gene therapy child from the Middle East and I had to make sure that the second eye surgery would not be cancelled since in these cases the timing within the two eyes is critical. Luckily, I was able to complete the treatment.
RL: What is your surgical protocol for your pediatric patients?
NB: Right now we are doing rapid testing for COVID before we take patients to the operating room. In the operating room we have changed our anesthesia protocols. Adult patients get MAC with nasal canals with very low flow oxygen and air suction place under the drapes. Every patient gets a surgical mask taped. For patients that require intubation, intubation and extubation occurs under a “tent” with a modified plastic viewing system.
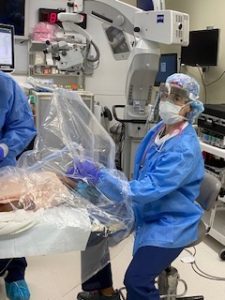
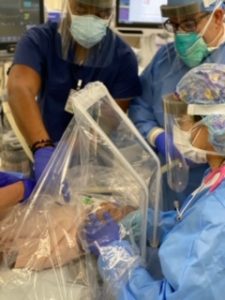
Intubation and extubation under the “tent”
Once intubated, they also get suction under the drapes. During intubation and extubation only the anesthesia team is in the room. Everyone in the room is using N95 masks with a surgical mask over it. The team (non-ophthalmologists) in the room are using facial shields. In the room, only the required personnel is present, no medical students, observers, etc.
RL: What is your PPE protocol for clinic and surgery?


Dr. Berrocal double masked for surgery Dr. Berrocal and Dr. Thomas Albini
NB: We use an N95 mask with a mask over it both in clinic and in the OR. Every patient that comes to clinic is given a mask. So far we have not done surgery on a known COVID + patient.
RL: What are you doing personally to relieve stress?
NB: Luckily, I have many hobbies that have been “on hold” during my full time working life, that are finally coming out. I actually like to cook (not every day my husband does everyday cooking) but now I find myself cooking more often and baking especially with my teenage kids. I started to paint again which I have not done in a long, long time and luckily I have a Peloton so I can ride with my friends around the country online. But, honestly what gives me the most peace is going to work and doing what I LOVE to do.
Dr. Nina Berrocal can be reached via e-mail – [email protected]

